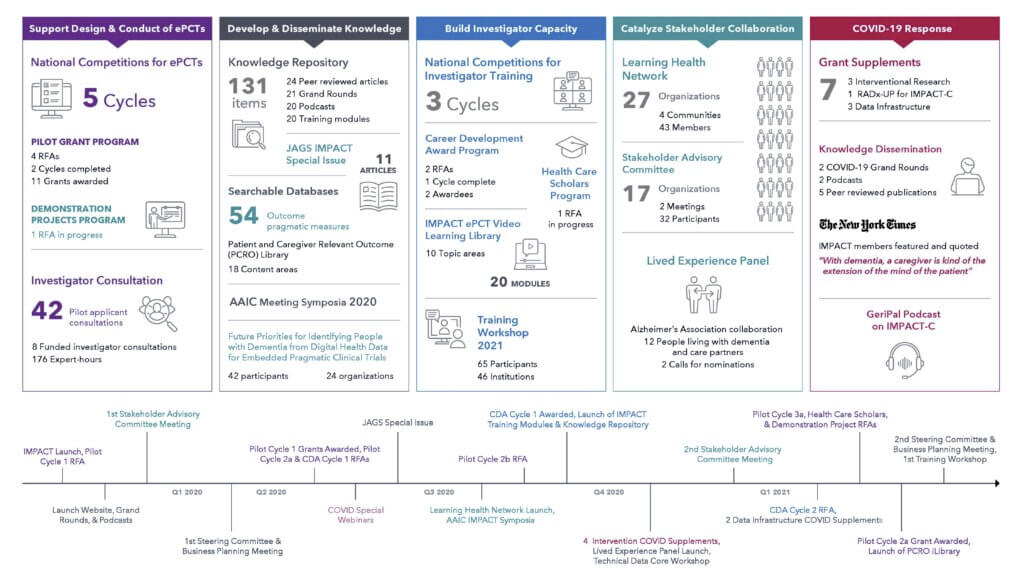
Asymptomatic and symptomatic infection rates fell dramatically after vaccinations in a large multi-state sample of nursing home residents, reported Wednesday in the New England Journal of Medicine
A study of more than 22,000 nursing home residents shows that the COVID-19 mRNA vaccines are highly effective under real-world conditions in reducing infection in this vulnerable population. The study, based at Brown University through a supplement award to the National Institute on Aging (NIA) IMbedded Pragmatic Alzheimer’s disease (AD) and AD-Related Dementias (AD/ADRD) Clinical Trials (IMPACT) Collaboratory, uses electronic health record data from Genesis HealthCare, one of the largest long-term care providers in the US. This is one of the first studies to report individual-level vaccine effectiveness data on nursing home residents, who were excluded from the vaccine clinical trials and often have reduced immune responses to vaccines.
The findings were shared as a research letter in the New England Journal of Medicine on May 19, and are attributed to a year-long collaboration between Brown University and Genesis HealthCare that has leveraged real-time clinical data to investigate COVID-19 outcomes in nursing homes. Led by Elizabeth White, PhD, APRN of the Center for Gerontology and Healthcare Research at the Brown University School of Public Health, the study team included Xiaofei Yang, ScM, Vincent Mor, PhD, and Stefan Gravenstein, MD, MPH from Brown University; and Carolyn Blackman, MD, and Richard Feifer, MD, MPH of Genesis HealthCare. Dr. Mor is one of two principal investigators of the IMPACT Collaboratory.
The study team examined clinical data from 280 nursing homes in 21 states. A total of 18,242 nursing home residents received at least one vaccine dose, and 13,048 of those received both doses as of February 15, 2021. An additional 3,990 residents were unvaccinated. Residents were observed for new infections through March 31, 2021. Residents underwent regular testing, and were assessed daily by nurses for new symptoms.
The incidence of asymptomatic and symptomatic infection fell for both vaccinated and unvaccinated residents over time. Of the 13,048 fully vaccinated residents, 38 (0.3%) developed incident infection more than 14 days after the second dose, but only 9 (0.1%) were symptomatic. Most infections were asymptomatic. The study results are in line with a recent CDC study of Chicago-area nursing homes, but expand upon those findings with a larger and more geographically diverse sample.
The reduced infections in unvaccinated residents suggest that robust resident and staff vaccine coverage, together with continued use of facemasks and other infection control measures, likely affords protection for small numbers of unvaccinated residents in congregate settings. Still, the continued observation of post-vaccine incident cases highlight the critical need to make vaccines and surveillance testing continuously available to nursing homes to mitigate future outbreaks.
“These findings clearly demonstrate the effectiveness and importance of vaccination among nursing home residents, particularly considering their frailty and weakened immune systems. Moreover, the data reinforce the need to maximize vaccine acceptance within this most vulnerable population” says Dr. Feifer, Chief Medical Officer for Genesis HealthCare.
Read the full letter and supplemental materials here.