September 1, 2020

A hurdle model is a modified count model that also assumes a relatively high frequency of zeros, but is set up as a two-stage data generation process rather than as a mixture distribution. In his most recent blog post, Keith Goldfeld, DrPH, MS, MPA of the IMPACT Design and Statistics Core discusses using a hurdle model in the context of planning a new study to address COVID-19 infection rates in nursing homes using much more aggressive testing strategies. Read the full blog post here.
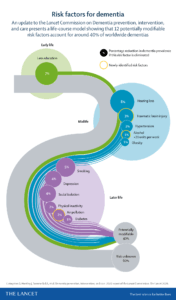 The Lancet Commission on dementia prevention, intervention, and care published a report July 30, 2020 that highlights recommendations for policy makers and individuals to help reduce dementia risk worldwide.
The Lancet Commission on dementia prevention, intervention, and care published a report July 30, 2020 that highlights recommendations for policy makers and individuals to help reduce dementia risk worldwide.
Eric B. Larson, MD, MPH, core leader of the IMPACT Health Care Systems Core and Laura Gitlin, PhD, FGSA, FAAN, core leader of the Implementation Core are among 28 internationally recognized dementia experts who contributed to the comprehensive report.
The report expands the number of modifiable risk factors from nine to 12, to now include head injuries in mid-life, excessive alcohol consumption in mid-life, and exposure to air pollution in later life. The Commission estimates that 40% of dementia cases could be prevented or delayed by targeting these 12 modifiable risk factors. The 2020 Lancet Commission update calls for nations and individuals to be ambitious about preventing dementia, and lays out a set of policies and lifestyle changes to help. Read https://hubs.ly/H0s-vHK0
Larson also answered questions from Kaiser Permanente Washington about the report. You can read the Q&A at this link.

May 11, 2020
 Kathleen Unroe, MD, MHA from the IMPACT Pilot Studies Core recently co-authored an editorial published in the Journal of the American Geriatrics Society. In it, they stated the benefits of collaboration between health systems and nursing facilities.
Kathleen Unroe, MD, MHA from the IMPACT Pilot Studies Core recently co-authored an editorial published in the Journal of the American Geriatrics Society. In it, they stated the benefits of collaboration between health systems and nursing facilities.
The editorial, "Time to Leverage Health System Collaborations: Supporting Nursing Facilities Through the COVID-19 Pandemic," was written in response to a paper published by a research team from the University of Washington. Dr. Unroe and her colleague Joshua Vest, PhD, MPH praise the work, which leveraged an existing university health system infrastructure to provide solutions and support to nursing homes during the outbreak. They believe the University of Washington's model demonstrates what is possible when investments are made in partnerships.
Read more about Dr. Unroe's editorial here.
IMPACT’s Multiple Principal Investigators Susan Mitchell, MD, MPH and Vincent Mor, PhD, together with Angelo Volandes, MD, recently published results of The Pragmatic Trial of Video Education in Nursing Homes (PROVEN) trial, a demonstration project under the NIH Health Care Systems Collaboratory.
PROVEN was among the first large-scale embedded pragmatic clinical trials conducted in nursing homes. The trial was conducted between February 1, 2016 and May 31, 2019 in 360 nursing homes (119 intervention and 241 control) owned by two for-profit corporations in 32 states. PROVEN tested the effectiveness of an advance care planning (ACP) video intervention, intended to help nursing home residents understand and chose their preferred goal of care. A suite of 5 different ACP videos were made available on tablet devices and online and offered to residents and their proxies at time of admission to the nursing home and then again every 6 months. Control nursing homes used usual advance care planning practices. The primary outcome was hospital transfers among long-stay (> 100 days) residents with advanced illness. Secondary outcomes included the proportion of those residents experiencing one or more hospital transfers, burdensome treatments, and hospice enrollment. Twelve month outcomes were measured for each resident. Data sources included Centers for Medicare & Medicaid Services Medicare claims and nursing homes’ electronic health records.
In this pragmatic cluster randomized trial, the PROVEN video intervention did not significantly reduce hospital transfers and burdensome treatments or increase hospice enrollment over 12 months among residents with advanced illness.
Overall intervention fidelity was low and highly variable across nursing homes, which may be one explanation of the negative findings. The low fidelity to the intervention highlights the challenge of implementing interventions in the nursing home environment and the need to ensure the highest level of engagement from key stakeholders, including front-line providers, when conducting pragmatic trials in this setting.
See the NIH HCS Collaboratory’s June 12, 2020, Grand Rounds webinar for a presentation of the PROVEN results: A Cluster Randomized Pragmatic Trial of an Advance Care Planning Video Intervention in Long-Stay Nursing Home Residents: Main Findings from the PROVEN Trial (Susan Mitchell, MD, MPH).
IMPACT Collaboratory co-principal investigator Vincent Mor, PhD and colleagues authored an opinion piece on June 25 in the Washington Post describing how research studies have shown that the key issue in managing infection rates of the virus within nursing homes is the rate of infection in the surrounding community.
Mor and his colleagues David C. Grabowski, professor of health-care policy at Harvard Medical School and R. Tamara Konetzka is a professor of health services research at the University of Chicago shared that all three had independently analyzed what determines whether a nursing home will see a coronavirus outbreak. All three research teams found that community infection rates where the nursing home was located was most strongly associated with high infection rates within the facilities.
“No care facility, no matter how excellent, can keep covid-19 away if it’s widespread in the areas where staff members live and work. To protect our most vulnerable citizens, we have to protect everyone,” said the authors in the article.
Read the full opinion piece in the Washington Post at this link.
Check out the latest blog post from Keith Goldfeld, DrPH, MS, MPA, executive committee member of the IMPACT Design and Statistics Core. Goldfeld considers the use of a permutation test for a small pilot study.
Link: https://www.rdatagen.net/post/permutation-test-for-a-covid-19-pilot-nursing-home-study/
AcademyHealth has developed a report focused on information needs of the health care and community organizations engaged in the COVID-19 response. The report is intended to inform decision-making of federal and foundation funders of health services research to guide investments in responsive research.
Read the full report and background information on the AcademyHealth website.